Teilnahmebedingungen für das Gewinnspiel “Brain Boost Event 2025 – Gewinne 2x Teilnahmeplätze für dich und deinen Lieblingskollegen in Seefeld”
Teilnahmebedingungen:

Cementing indirect restorations can be tricky – learn how to identify pitfalls, minimize flaws, streamline your procedure and achieve long term restorative success.
The cementation of indirect restorations is a critical procedure step with a huge impact on the long-term success of the prosthetic work. In order to avoid early failures, it is essential to identify potential sources of error – and to develop strategies that are as error-proof as possible. My personal experience from more than 100 training courses in dental offices shows that everywhere around the globe, individuals placing indirect restorations tend to make similar mistakes, and that the great majority of them are easily preventable. Take a closer look at common cementation pitfalls that could lead to failure, how to overcome them and ultimately, reach long-term success.
Errors and mistakes in the cementation procedure tend to fall in these four categories:

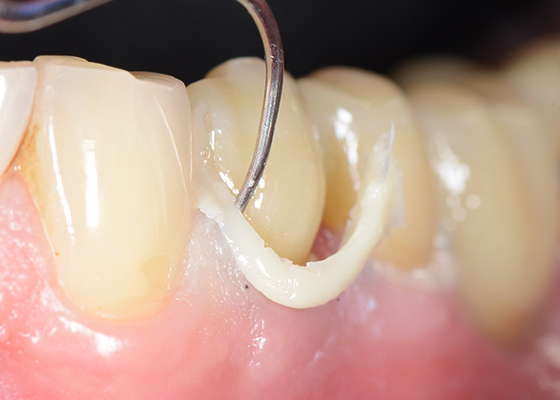
Cement layer with voids visible upon removal of a metal-ceramic restoration placed by another dental office. (Image courtesy of Frank Tussing, Gießen, Germany)
Who takes delivery of the indirect restorations arriving from the dental laboratory? Who brings them to the treatment unit? Does anyone touch them with their fingers, and if so, which measures are taken to clean the contaminated restorations afterwards? Where and under which storage conditions are the cements kept until needed? And who is responsible for exchanging the automix syringe’s mixing tip and checking the mix quality prior to cement application?
Organization is a prerequisite for creating a streamlined, error-proof cementation procedure: it is essential that all organizational tasks are clearly allocated to specific members of the practice team. At the same time, it is important for more than one person to know what to do – in order to avoid confusion whenever the responsible staff member is unavailable. Simply put: the processes need to be standardized from the beginning, and the same protocols should be valid for all teams within one dental office.
The questions asked above highlight the most critical factors that might compromise the quality of the cement layer. Touching a restoration with bare fingers, for example, increases the risk of infection and could compromise the bond strength. After being touched, just as after every try-in, the restoration needs to be cleaned with sodium hypochlorite for decontamination. A better strategy, however, is to avoid touching a restoration without gloves.
Storing a cement at temperatures higher than recommended will shorten the product’s shelf life. Using dual-cure or self-cure cements in this warmer-than-recommended state reduces working time. Lower-than-recommended storage temperatures have no negative impact on the product’s performance; however, the cements should reach the recommended temperature range before use to avoid any change in viscosity. Providing controlled storage conditions at room temperature makes it easier to ensure ideal viscosity, extrusion force, and working time when needed – in addition to a long shelf life.
In the context of exchanging the automix syringe’s mixing tip, one step is sometimes skipped: checking the mix quality by dispensing a small amount of material on a mixing pad. If this step is not performed, an inhomogeneous mixture or asynchronous flow will remain unnoticed – and will likely compromise the quality of the bond.

Make sure to always wear gloves when touching a restoration.

Check the quality of the mixture every time before applying the resin cement.
With essentially three different cement classes at hand, it is necessary to select the most suitable solution for the restorative material in use, the preparation design and the moisture control options. Due to their low bond strength, easy-to-use and moisture-tolerant conventional cements are only suited for clinical cases with a retentive preparation design and restorations made of metal or high-strength ceramics. Resin cements paired with a separate adhesive, on the other hand, provide the highest possible bond strength, but there is a tradeoff: they require a multi-step procedure and a dry working field. Consequently, they are recommended for the most demanding cases with low-strength restorative materials and non-retentive designs – but only if moisture control is possible. Self-adhesive resin cements provide a happy medium, combining both ease of use and reliable bond strength. These products are highly versatile and used for a wide range of indications.
In the worst-case scenario, making the wrong cement choice will lead to insufficient bond strength and ultimately to restoration failure. You can simplify your workflow by using a new universal cement class and accompanying adhesive: 3M™ RelyX™ Universal Resin Cement and 3M™ Scotchbond™ Universal Plus Adhesive. The cement produces the highest bond strength when combined with the adhesive, but can also be used as a standalone solution due to its self-adhesive properties. Therefore, you can confidently place it on the tray for all adhesive and self-adhesive resin cement indications.
Any manipulation of the prepared tooth structure or restoration might affect the performance of the cement and the final restoration. Errors in a core build-up procedure could compromise the stability of the abutment tooth and the quality of the bonding surface. An improperly designed temporary might lead to pressure sores and inflammation of the surrounding soft tissue. Any resulting swelling, bleeding, etc. could challenge the dental practitioner during restoration placement and might negatively affect the performance of the cement. Using a temporary cement that contains eugenol is risky, as eugenol residues will decrease the bond strength. To completely remove the eugenol, it is necessary to clean with hydrogen peroxide, which often produces hypersensitivities. Other substances that could potentially affect bond quality include the selected fit checking material and desensitizers.

Production of a temporary bridge made of 3M™ Protemp™ 4 Temporization Material with well-designed margins.

Use of Fit Checker™ Advanced Blue (GC Corporation) to assess the fit of a zirconia restoration. (Image courtesy of Hans-Jürgen Stecher, Germany)
The pretreatment and cementation protocols depend on the selected restorative material and the selected cementation procedure. Since glass-ceramic bonding surfaces need to be pre-treated with hydrofluoric acid, while zirconia surfaces require sandblasting, it is essential for your whole team to be well-informed about the restorative material in use – as well as whether the laboratory technician has already pre-treated the surfaces. As cleaning and reconditioning is always necessary after intraoral adjustments, it might be preferable to carry out the pretreatment measures in the dental office after try-in. This prevents over-conditioning and a structural weakening of the restorative material. Opting for the right cleaning solution for the restoration is also important. For example, cleaning zirconia with phosphoric acid is contraindicated whenever a phosphate-based cement or adhesive is used, as the phosphoric acid blocks the binding sites of the ceramic and impairs bond strength.
Learn more about ensuring proper pretreatment: Overview of Existing Pretreatment and Cementation Workflows.
When applying dual-cure cements, timing and the potential impact of ambient light should be considered. Both factors can have an effect on the working time (as can the temperature of the cement at the time of application). Light plays a decisive role for the adhesive as well: if stored in an open vessel for several minutes, the adhesive’s properties might change. During cement application, voids are a common issue that could compromise the quality of the bond and prevent a complete seal to the underlying tooth structure. When it comes to excess removal, common errors result from the formation of an oxygen inhibited layer or manipulation of the restoration, which might lead to lower bond quality or a malpositioned restoration, respectively. The latter might also be the result of an insufficient cure, whether a light-cure or dual-cure cement.

Pre-treat glass-ceramic restorations with hydrofluoric acid gel after try-in. (Image courtesy of Prof. Jan-Frederik Gueth, Munich, Germany)

Pre-treat zirconia restorations by sandblasting. (Image courtesy of Prof. Jan-Frederik Gueth, Munich, Germany)

Preferably remove excess cement after tack-curing.
As the saying goes, “the devil is in the details.” It is often the small and avoidable errors or imprecisions in the cementation workflow that cause issues like an incomplete marginal seal, decreased bond strength or otherwise impaired quality of the cement layer – all of which increase the probability of restoration failure. How do you keep these errors from creeping in? By being alert for the potential pitfalls of cementation, and by standardizing procedures across your practice. These proactive steps will help you nail the details – and that will pay off in the long run.
For a closer look at cementation, download our white paper: Demystifying cementation: Master the vital principles every dentist should know.

How do you motivate your patients? Discover how caries risk assessments and motivational interviewing tactics can help you connect with…

Caries is a complicated multifactorial disease. In this two-part series, explore how caries risk assessments can help improve evaluation and…