What is the name of the patron saint of dentists?
Brain of the Week – History

Esthetic anterior indirect restorations can be difficult, but they don’t have to be. Streamline your decision-making process and set yourself up for success from the start – and make the best choice for every case.
1. Wear of human enamel opposing monolithic zirconia, glass ceramic, and composite resin: An in vitro study, The Journal of Prosthetic Dentistry, Volume 112, Issue 5, 2014, Pages 1141-1150, ISSN 0022-3913.
2. Gou M, Chen H, Kang J, Wang H. Antagonist enamel wear of tooth-supported monolithic zirconia posterior crowns in vivo: A systematic review. J Prosthet Dent. 2019 Apr;121(4):598-603. doi: 10.1016/j.prosdent.2018.06.005. Epub 2018 Dec 1. PMID: 30509545.
3. Lawson NC, Janyavula S, Syklawer S, McLaren EA, Burgess JO. Wear of enamel opposing zirconia and lithium disilicate after adjustment, polishing and glazing. J Dent. 2014 Dec;42(12):1586-91. doi: 10.1016/j.jdent.2014.09.008. Epub 2014 Sep 23. PMID: 25257823.

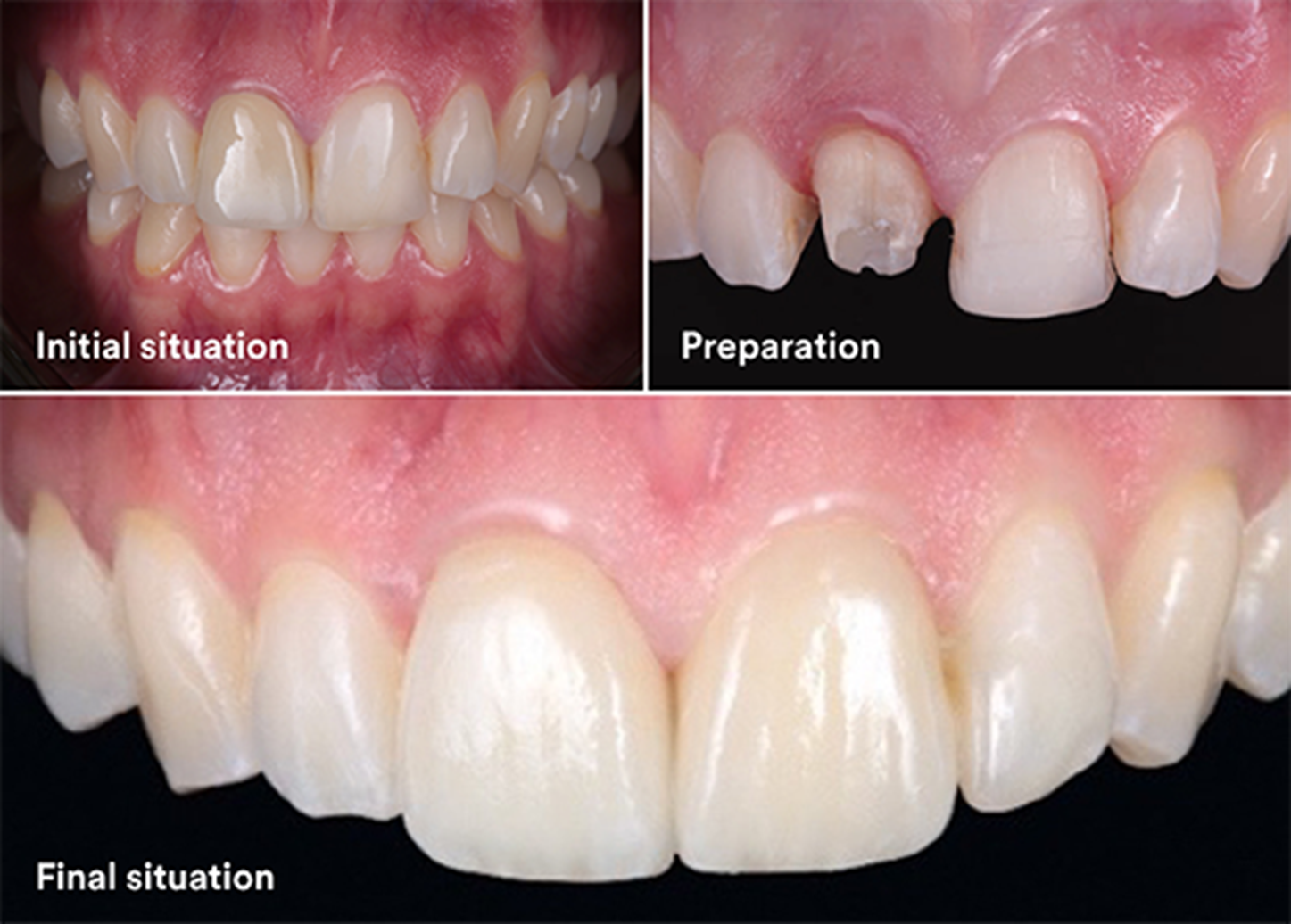
Initial situation and after preparation for both a crown and a veneer restoration
Restoring anterior incisors with varying treatment needs is probably one of the most challenging procedures in dentistry. There are a wide range of treatment options but only a few materials will provide outstanding esthetic results and mimic natural tooth structure in detail, shade and translucency. Plus, functional parameters and the condition of the remaining hard tissues sometimes require using different materials side by side to balance strength with esthetics.
In order to make the best decision for each case, one needs to fully understand the material options and their individual pros and cons, as well as how they’ll fit the needs of the specific clinical situation. Needless to say, deciding which material to use may be just as difficult as the procedure itself! This is where establishing a clear decision-making protocol can come in handy.

There are three main restorative materials to choose from, namely: composites/hybrids, glass ceramics and oxide ceramics, as well as combinations of these materials, such as PFM (porcelain-fused-to-metal) and veneered ceramics. All of these restorations may be fabricated chairside or in a laboratory. Since CAD-CAM (computer-aided-design and computer-aided-manufacturing) dentistry has grown in popularity and is used quite frequently, this will be the focus here.
Composite and hybrid restorative materials are a growing category of restorative materials but aren’t popularly used in the anterior region for a number of reasons, including the misconception that they aren’t strong or esthetic enough to support the region, the need for more aggressive preparation due to higher material thickness requirements, and a lack of insurance coverage. However, new formulations and techniques have made these materials far more versatile, as well as a viable and beneficial choice for a number of clinical situations. These modern materials address past issues with improved mechanical and esthetic properties as well as improved handling, in turn, creating new opportunities to work more conservatively.
Glass ceramic restorative materials are an excellent choice when high esthetics are required. Feldspathic porcelain and lithium disilicate are the most commonly used materials in this material class as they provide excellent translucency and esthetic qualities. They cover a variety of clinical situations with a range of monochromatic to polychromatic blocks in both high translucency and low translucency options. And while milling glass ceramics is not as easy as milling composite, it can still be performed successfully. Bonding is predictable, and while glass ceramics are weaker than zirconium oxide, their strength is sufficient for anterior restorations.
The main disadvantages of glass ceramics are their accompanying costs for both the patient and the lab. In addition, the extra time needed to bond ceramic crowns can also increase costs and impact your bottom line.
Zirconium oxide restorative materials are used for a fair share of anterior restorations due to their mechanical strength and advanced esthetics. This high mechanical strength allows for thinner restoration walls, which helps improve esthetics and preserve more healthy tooth structure – particularly when used for monolithic restorations (see table below). It’s a naturally tooth-colored material that can also be veneered with porcelain to further enhance the esthetics of the final restoration. The use of monolithic restorations is often limited by esthetic appearance, especially when only a single tooth is restored, and neighboring natural teeth will remain untouched in the visible area. Since porcelain layering is rarely associated with chipping in the anterior region, it’s a good option to ensure esthetic longevity.
And while there’s a misconception that harder materials translate to increased friction and more wear to adjacent teeth, the truth is that polished zirconia has been shown to have less abrasive effect than glass ceramics!1-3 With all this in mind, zirconium oxide is not as esthetic as glass ceramics – and may be difficult to color match, depending on the material chosen.
Ensuring a successful esthetic outcome not only means selecting the optimal material and shade, but also ensuring accurate preparation guidelines and communicating effectively with laboratory technicians. With everything above in mind, how do you decide which material to use?


Ideal crown preparation design in incisors to realize ideal material thicknesses.
To give clinicians an orientation on indication-specific material selection and clinical tips for their successful and highly efficient use, 3M and dental experts developed a guideline to help simplify decision making – every step of the way. The guideline emphasizes simplicity, and it starts with selecting a technique that follows three basic rules. The chosen technique should be:
With these principles in mind, we developed recommendations for the most critical aspects of indirect restorative procedures – including choosing the ideal material for each case. In order to select the best material, multiple clinical, esthetic and mechanical factors need to be considered. While esthetic demands are mainly based on the location of the restoration, the strength required from the material is determined by the position, substrate, indication and prep design. By going through each of these factors, one can find the best possible option for the case at hand:

Consider the following case, in which a 24-year-old patient wanted to enhance the esthetics of their upper central incisors. This included an old, discolored zirconia crown on tooth 21 and an inadequate cervical margin. Tooth 11 had old composite restorations.
With so many different needs within the same area, it can be difficult to make a solid plan. But if we approach the situation using the previously detailed factors, we can narrow down which material is the best choice – or choices – for this case:
As for the crown, since the tooth had previously been restored with zirconia and simply needed replacement, zirconia was deemed the best option.
A retentive prep for a crown generally allows for any type of cement, as no extra bond strength is needed due to the mechanical retention provided by the preparation design. So, retentive preps can be cemented using a conventional cement, without a bonding agent (like a glass ionomer cement or a resin modified glass ionomer cement).
A non-retentive prep for a veneer needs a cement with high bond strength capability so that the restoration will bond to the tooth.
All of these factors combined point to a combination of glass ceramics and veneered zirconia. Not only do these materials fulfill the high esthetic demands of the area, but they also account for the unique mechanical needs of the case.

Another critical factor to take into account: bonding possibilities. Bonding or cementing should be considered from the very start of treatment but is often left until the last possible moment, if not overlooked entirely. Dental materials are not one size fits all when it comes to adhesion, e.g., a material can’t be cemented if bonding is required. That’s why it’s important to know your material and its specific bonding or cementation needs.
For example, if isolation is going to be difficult, a combentionally cementable restoration should be considered. Conventional cements are more moisture tolerant than the other resin cements, which makes them a solid choice when good isolation is not possible. In terms of the case above, we need to consider a zirconia crown and glass ceramic veneers:
As demonstrated in this case, different materials can be used on neighboring teeth without issue, as they can still show perfect esthetic results regardless of their inherent differences.
It’s important to keep in mind that all the effort you put into selecting the right material is only as good as your communication with the lab. The lab can only work with what you give them – so make sure you provide as much detail as possible. Plus, not all labs will offer all solutions, so it’s vital you know what the lab you’re using is capable of and if they can meet your, your procedures’ and your patients’ needs.
Selecting the right material for the anterior can be complicated – but by taking a step back and streamlining your decision-making process, you can take the stress and guesswork out of your day and spend more time restoring smiles.

Brain of the Week – History

Discover the latest updates to our software for your digital orthodontic treatments.
SAVE THE DATE!